Chronic kidney disease cats signs can be easy to miss because many cats look “mostly normal” while kidney function is gradually changing. Increased thirst, larger urine clumps, weight loss, appetite changes, vomiting, and poor coat quality may look like aging at first, but together they deserve veterinary attention.
This article is not meant to diagnose kidney disease at home. A cat cannot be confirmed to have chronic kidney disease from symptoms alone. Diagnosis usually requires a veterinary exam, bloodwork, urinalysis, urine specific gravity, blood pressure assessment, and sometimes repeat testing.
When Oliver turned ten, I started watching his water bowl and litter box more carefully. Not because he had kidney disease, but because senior cats benefit from earlier detection. The goal is not to panic over every change. The goal is to notice patterns early enough to ask the right questions at the clinic.
Quick Answer: What Are the Earliest Chronic Kidney Disease Cats Signs?
The most common chronic kidney disease cats signs include increased thirst, larger or more frequent urine clumps, reduced appetite, gradual weight loss, nausea, poor coat quality, and vomiting. These signs do not prove kidney disease by themselves, but they are strong reasons to schedule a veterinary exam, especially in cats over seven years old.
Early screening often includes bloodwork, SDMA, creatinine, BUN, phosphorus, urinalysis, urine specific gravity, and blood pressure. According to ISFM and IRIS guidance, staging and treatment decisions should be based on veterinary testing, not symptoms alone.
Important Veterinary Note
This guide is for general education only and is not a substitute for veterinary diagnosis or treatment. If your cat stops eating, cannot keep water down, seems weak, hides suddenly, strains to urinate, produces no urine, vomits repeatedly, collapses, or appears painful, contact a veterinarian or emergency clinic promptly. Do not start a renal diet, phosphorus binder, supplement, appetite stimulant, or fluid therapy without veterinary guidance.
Why Early Kidney Changes Are Often Missed
The clinical reality that makes chronic kidney disease cats signs so difficult to catch early is captured in what nephrologists call the 75% Rule: cats do not show obvious clinical signs of kidney insufficiency until approximately 75% of their functional nephron mass has been lost.
Nephrons are the functional filtering units of the kidney — each kidney contains hundreds of thousands of them, and they do not regenerate once lost. The surviving nephrons compensate for lost colleagues by increasing their individual filtration rate — a process called compensatory hypertrophy that is effective at maintaining outward clinical normality but that also accelerates the rate of nephron exhaustion in the remaining population.
This compensatory mechanism is simultaneously the reason cats survive early CKD so well and the reason the disease is so diagnostically elusive in its early stages.
What “75% loss before symptoms appear” means in practice:
- A cat who appears completely normal may have lost half their functional kidney tissue
- The Sub-clinical Phase of CKD — active disease with no detectable clinical signs — can last years
- By the time traditional laboratory markers like creatinine become elevated, the disease is already well-established
- The window for maximum therapeutic impact is almost entirely within the period when most owners have no idea anything is wrong
Renal health is the single most important metric for maximizing how long your indoor cat will live — and the cats who live longest with CKD are almost universally those whose disease was detected earliest, before the clinical signs that most owners are watching for have appeared.

7 Chronic Kidney Disease Cats Signs to Watch For
Sign 1: The Water Bowl Obsession (Polydipsia)
Increased water consumption — polydipsia — is the chronic kidney disease cats sign that owners most commonly notice first, though they frequently do not recognize it as a medical indicator until it becomes dramatic.
Diseased kidneys lose the ability to concentrate urine efficiently — a process called isosthenuria or hyposthenuria depending on severity — and the body responds by driving increased water intake to compensate for the fluid losses through inappropriately dilute urine. The thirst increase is the body’s attempt to maintain fluid balance in the face of a kidney that is no longer conserving water adequately.
What to watch for:
- Visiting the water bowl or fountain noticeably more frequently than previous baseline
- Drinking from unusual sources — sink drips, bathtub residue, glasses left on counters
- Longer duration drinking sessions than previously observed
- Vocalizing near empty water bowls
How to quantify it: Measure your cat’s daily water intake by filling the bowl or fountain reservoir to the same level each morning and measuring what remains 24 hours later, accounting for any water added. A 10-pound cat consuming more than 50ml of water per kilogram of body weight per day is showing clinically significant polydipsia.
Sign 2: The Full Litter Box (Polyuria)
Polyuria — excessive urine production — is the physiological partner to polydipsia and is one of the most reliable early chronic kidney disease cats signs for owners willing to monitor their litter box with clinical attention.
A cat with normal kidney function produces concentrated, dark yellow urine in relatively modest volumes. A cat with declining kidney function produces large volumes of pale, dilute urine that creates larger-than-normal litter clumps and requires more frequent litter box scooping to maintain acceptable conditions.
Monitoring litter box clumps is a non-negotiable part of a senior cat wellness routine at home — the size, color (observable before clumping in non-clumping litter), and frequency of urination provide daily data points about kidney function that no clinic visit can replicate because they represent the cat’s normal-environment output rather than a stress-affected clinic sample.
What to watch for:
- Clump size that is noticeably larger than your established baseline
- More clumps per day than your established baseline
- Litter box that fills faster than usual
- Pale, almost colorless urine visible in non-clumping litter
Sign 3: The Picky Eater Shift (Reduced Appetite)
Cats with CKD accumulate uremic toxins — the waste products that healthy kidneys filter from the blood — and these toxins cause nausea, altered taste perception, and gastrointestinal inflammation that combine to produce a characteristic appetite pattern: the cat who used to eat enthusiastically now approaches the bowl, sniffs, and walks away.
This is frequently misinterpreted as the cat being “bored with their food” and leads owners to rotate through multiple food options — which temporarily restores eating behavior and masks the underlying medical cause.
What distinguishes CKD-related appetite reduction from simple food preference:
- The change is progressive — food that worked three weeks ago is increasingly rejected
- The cat shows interest in food (approaching the bowl) but does not eat — nausea rather than disinterest
- Weight loss occurs despite apparently normal or only mildly reduced intake
- The cat may eat small amounts frequently rather than completing normal meal portions
Sign 4: The Weight Loss That Hides in Plain Sight
Muscle wasting — cachexia — is one of the most significant and most consistently missed chronic kidney disease cats signs because it happens slowly enough that daily observers do not perceive the cumulative change.
CKD-associated weight loss occurs through several mechanisms: reduced caloric intake from nausea and appetite suppression, increased protein catabolism as the body compensates for metabolic derangements, and loss of lean muscle mass that is characteristic of uremic syndrome.
Why this sign is missed:
- Owners who see their cat daily do not perceive gradual changes the way a veterinarian who examines the cat every six months does
- A fluffy long-coated cat can lose significant muscle mass that is completely concealed beneath the coat
- Weight loss is frequently normalized as “getting older” rather than recognized as a clinical sign
The home monitoring tool: Weigh your cat monthly on a kitchen scale from the age of 8 onward. Any weight loss exceeding 10% of baseline body weight over a 3–6 month period warrants veterinary evaluation regardless of coat appearance.
For a broader monthly monitoring routine, read our guide on how to do a cat health check at home.
Sign 5: The Staring at Water Posture (Nausea and Malaise)
One of the chronic kidney disease cats signs that experienced cat owners sometimes notice and rarely know what to make of is what I think of as the staring at water posture: the cat stands over the water bowl or sits very close to it, oriented toward it, but does not drink. The cat may sit in this position for several minutes before moving away without drinking.
This behavior reflects the complex interaction between nausea (which creates an aversion to drinking despite physiological thirst), the increased thirst drive of polyuria, and the confusion of receiving competing signals simultaneously. The cat is drawn to water by thirst but repelled by nausea at the moment of contact.
Additional malaise-associated postures:
- Sitting in a hunched, slightly tucked position with elbows drawn inward
- Spending increased time pressed against cool surfaces — tile floors, bathroom basins — as CKD-associated anemia reduces heat tolerance
- Decreased interest in the environment — less window-watching, less response to sounds and movement that previously generated interest
Sign 6: The Coat Quality Collapse
A cat’s coat is a real-time indicator of systemic health, and the coat changes associated with chronic kidney disease cats signs are visible to an attentive owner months before more obvious clinical signs appear.
CKD-related coat deterioration occurs because reduced protein absorption and increased protein catabolism deprive the rapidly growing hair follicle cells of the amino acid substrates they require. The result is a coat that loses its reflective quality, feels different in texture (coarser or more brittle), and begins to appear unkempt even in cats who are still grooming normally.
Coat changes to monitor:
- Loss of the healthy sheen that reflects light across the coat surface
- Dry, brittle, or harsh texture on palpation that was previously soft
- Increased visible dandruff — reduced skin oil production from nutritional deficiency
- In long-coated cats, mats appearing in areas the cat can reach — reduced grooming drive combined with coat texture change
Sign 7: The Episodic Vomiting Pattern
Occasional vomiting is so normalized in cat ownership that it is rarely flagged as a chronic kidney disease cats sign — and this normalization causes meaningful diagnostic delays in cats whose vomiting is not hairball-related but uremia-related.
Uremic gastritis — the inflammation of the gastric mucosa caused by accumulating uremic toxins — produces a vomiting pattern that is distinguishable from hairball vomiting by several characteristics:
CKD-associated vomiting characteristics:
- Content: Bile, foam, or undigested food rather than tubular hairball material
- Frequency: 2–4 times per week, progressive over months rather than episodic
- Timing: Often in the morning or between meals — gastric acid accumulation when the stomach is empty
- Association: Frequently accompanied by the other chronic kidney disease cats signs described above
- Response to hairball treatment: No improvement with lubricating gels or fiber supplementation
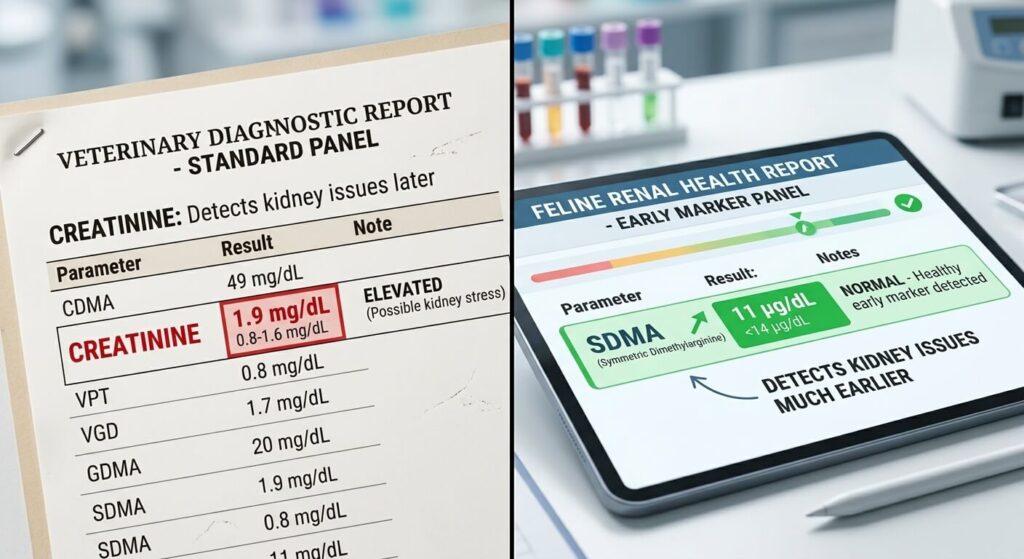
SDMA, Creatinine, and Urinalysis: How Vets Screen for CKD
The most significant advancement in feline CKD detection in the last decade is the development and clinical adoption of SDMA Testing — the measurement of Symmetric Dimethylarginine, a biomarker of glomerular filtration rate that becomes elevated earlier in the disease process than the traditional creatinine marker.
Understanding the difference:
Creatinine is a muscle metabolism byproduct that the kidneys filter from the blood. It becomes elevated in bloodwork when approximately 75% of kidney function has been lost — the same threshold at which clinical signs appear. A cat with normal creatinine may have already lost two-thirds of their functional kidney tissue.
SDMA is a methylated arginine amino acid produced at a constant rate by all cells and cleared exclusively by the kidneys. It becomes elevated when approximately 40% of kidney function has been lost — meaning it can flag CKD years before creatinine rises and before any chronic kidney disease cats signs are detectable by the owner or on physical examination.
The clinical impact of SDMA testing:
| Parameter | Creatinine | SDMA |
|---|---|---|
| Kidney function lost at elevation | ~75% | ~40% |
| Lead time over clinical signs | Minimal | Potentially 2–4 years |
| Muscle mass dependence | Significant | Minimal |
| Availability | Standard panel | Now included in most comprehensive panels |
The muscle mass dependence of creatinine is a specific problem in elderly cats: a cat with significant muscle wasting — itself a chronic kidney disease cats sign — may have a falsely normal creatinine because they have less muscle to produce creatinine, even while their kidney function is severely compromised. SDMA Testing is not subject to this confounding variable.
The International Renal Interest Society (IRIS) Staging System is the current standard for staging feline CKD severity and guiding treatment decisions:
| IRIS Stage | Creatinine (mg/dL) | SDMA (µg/dL) | Clinical Status |
|---|---|---|---|
| Stage 1 | < 1.6 | 18–25 | Non-azotemic; SDMA elevated |
| Stage 2 | 1.6–2.8 | 25–38 | Mild azotemia; may have subtle signs |
| Stage 3 | 2.9–5.0 | 38–54 | Moderate azotemia; clinical signs present |
| Stage 4 | > 5.0 | > 54 | Severe azotemia; significant clinical signs |
My recommendation for Oliver — and every cat over 7: Annual comprehensive bloodwork including SDMA Testing from age 7 onward, moving to biannual testing at age 10. The cost of this testing is the most financially effective preventive health expenditure available for senior cat owners, because Stage 1 and Stage 2 CKD management is dramatically less expensive and dramatically more effective than Stage 3 and Stage 4 crisis management.
Kidney care can become expensive over time, especially if repeat bloodwork, urine testing, blood pressure checks, prescription food, medication, or emergency visits are needed. For the cost-planning side, read our guide on whether pet insurance is worth it for indoor cats.
For senior cats, kidney screening fits best into a consistent wellness routine. See our guide to the annual vet visit for an indoor cat for what to review before each appointment.
Diet and Phosphorus: What to Discuss With Your Vet
Once chronic kidney disease is confirmed, diet becomes one of the most important management conversations to have with your veterinarian. For many CKD cats, veterinary renal diets are designed to manage phosphorus, protein balance, calories, sodium, potassium, and palatability. But the right diet depends on the cat’s stage, blood phosphorus level, appetite, hydration, body condition, and other diseases.
Do not switch a cat to a renal diet just because you notice possible chronic kidney disease cats signs. A cat who is losing weight or eating poorly may need calories and appetite support before diet restriction. Your veterinarian can use bloodwork, urinalysis, blood pressure, and IRIS staging to decide whether a renal diet, phosphate binder, fluids, nausea medication, or appetite support is appropriate.
Why phosphorus matters:
Healthy kidneys filter dietary phosphorus efficiently. Diseased kidneys accumulate phosphorus in the blood — a condition called hyperphosphatemia. Elevated blood phosphorus triggers the secretion of Fibroblast Growth Factor 23 (FGF-23) and Parathyroid Hormone (PTH), both of which cause additional kidney damage in a self-amplifying cycle. Phosphorus Restriction interrupts this cycle and is the dietary intervention with the strongest evidence for slowing CKD progression.
Practical dietary guidance:
- Prescription renal diets (Hills k/d, Royal Canin Renal, Purina NF) are formulated with specific Phosphorus Restriction and protein modification — these diets have controlled clinical trial evidence supporting their ability to extend survival in CKD cats and should be the first dietary recommendation from your veterinarian
- High phosphorus foods to avoid: dairy products, fish (particularly sardines, tuna, and mackerel), organ meats (liver, kidney), and any food with phosphate salt additives listed as ingredients
- Protein quantity: CKD cats require careful protein calibration — too little protein worsens muscle wasting, too much accelerates uremic toxin accumulation; prescription renal diets are formulated to this specific balance
- Hydration priority: Wet food as the primary diet is strongly recommended — dehydration concentrates uremic toxins and accelerates nephron damage

Phosphate binders — medications that bind dietary phosphorus in the gut before it is absorbed — are frequently prescribed alongside dietary Phosphorus Restriction when dietary modification alone cannot achieve target blood phosphorus levels. These are prescription products requiring veterinary guidance for appropriate dosing.
FAQ
Can you reverse kidney disease in cats?
No — Chronic Kidney Disease (CKD) involves the irreversible loss of functional nephrons, and current veterinary medicine has no mechanism to regenerate lost kidney tissue. What is possible, and what makes early detection of chronic kidney disease cats signs so clinically meaningful, is significantly slowing the progression of the disease.
Cats diagnosed at IRIS Stage 1 or Stage 2 who receive appropriate dietary management, phosphorus restriction, blood pressure control where indicated, and regular monitoring can maintain stable kidney function for years. The distinction between “reversible” and “manageable” is critical — CKD cannot be cured, but its trajectory can be profoundly altered by early intervention.
What is the best food for a cat with early kidney disease?
Veterinary prescription renal diets — Hills Prescription Diet k/d, Royal Canin Veterinary Renal, and Purina Pro Plan Veterinary NF — are the evidence-based recommendation for cats with confirmed CKD at any stage, because these diets have been specifically formulated for Phosphorus Restriction and appropriate protein content, and they have controlled clinical trial data supporting their efficacy.
The wet food formulations of these diets are preferred over dry formulations because hydration support is as therapeutically important as phosphorus control in CKD management. For cats who refuse prescription renal diets — not uncommon, as appetite suppression is itself one of the chronic kidney disease cats signs — your veterinarian can guide a pragmatic approach balancing palatability and nutritional management.
How do vets confirm chronic kidney disease in cats?
Veterinarians usually confirm chronic kidney disease by looking at a pattern of findings, not one symptom alone. Testing may include bloodwork, SDMA, creatinine, BUN, phosphorus, urinalysis, urine specific gravity, urine protein testing, blood pressure, and repeat testing over time. Your vet may also check for dehydration, urinary tract infection, hyperthyroidism, high blood pressure, and other conditions that can affect kidney values.
Should I change my cat’s food if I suspect kidney disease?
No, not without veterinary guidance. A renal diet can be very helpful for cats with confirmed CKD, but appetite, weight, hydration, phosphorus levels, and disease stage matter. If your cat is eating poorly or losing weight, the first priority may be diagnosis, nausea control, hydration support, and maintaining calories. Call your veterinarian before changing food, adding supplements, or using phosphorus binders.
How long can a cat live with chronic kidney disease?
Survival time in feline CKD varies enormously with stage at diagnosis, individual cat response to management, and the presence or absence of concurrent diseases. Published median survival times from IRIS staging data: Stage 1 — potentially years with appropriate management; Stage 2 — median approximately 1,151 days (roughly 3 years) in managed cats; Stage 3 — median approximately 778 days (roughly 2 years) in managed cats; Stage 4 — median approximately 103 days.
These are median figures — individual cats significantly exceed and fall below these numbers. The most important variable in survival duration is when chronic kidney disease cats signs are recognized and management begins, which is why the SDMA Testing advancement is so clinically significant — it shifts the intervention point earlier, when the survivability curve is most favorable.
Final Thoughts
Chronic kidney disease cats signs are worth taking seriously, but they should not be used as a home diagnosis. The useful pattern is not one isolated clue. It is a combination of changes: more drinking, larger urine clumps, weight loss, appetite shifts, vomiting, coat decline, and reduced energy.
Oliver’s most recent bloodwork was normal, and I am grateful for that. I still watch his water intake, litter box, weight, appetite, and annual lab results because senior-cat health is easier to protect when changes are noticed early. That is the point of monitoring: not fear, but earlier conversations with the veterinarian.
References
- Sparkes, A. H., Caney, S., Chalhoub, S., Elliott, J., Finch, N., Gajanayake, I., Langston, C., Lefebvre, H. P., White, J., & Quimby, J. (2016). ISFM Consensus Guidelines on the Diagnosis and Management of Feline Chronic Kidney Disease. Journal of Feline Medicine and Surgery, 18(3), 219–239.
- International Renal Interest Society. IRIS Staging of CKD.
- Hall, J. A., Yerramilli, M., Obare, E., Yerramilli, M., & Jewell, D. E. (2014). Comparison of serum concentrations of symmetric dimethylarginine and creatinine as kidney function biomarkers in cats with chronic kidney disease. Journal of Veterinary Internal Medicine, 28(6), 1676–1683.
- American Animal Hospital Association. (2023). 2023 AAHA Senior Care Guidelines for Dogs and Cats.

-300x169.png)
-300x169.png)
