Cat vomiting vs hairball confusion is common because both can involve retching, noise, mess on the floor, and a cat who seems normal afterward.
The difference matters because a true hairball is usually a firm, tube-shaped mass of fur, while vomiting may contain food, liquid, bile, foam, or blood. A single hairball in a bright, comfortable cat is often a monitoring situation. Repeated vomiting, unproductive retching, blood, lethargy, appetite loss, or signs of pain should be treated as a reason to contact your veterinarian promptly.
This guide shows you how to compare shape, contents, color, frequency, and after-vomiting behavior so you can describe the episode clearly to your vet and know when it is not “just a hairball.”

Quick Answer: Cat Vomiting vs Hairball
Cat vomiting vs hairball differences usually come down to shape, contents, effort, and what your cat does afterward. A hairball is often cylindrical, firm, and visibly made of packed fur. Vomit is more likely to be liquid, foamy, bile-colored, bloody, or mixed with food.
If your cat produces one clear hairball and then eats, drinks, grooms, and behaves normally, monitor closely and work on prevention. If your cat vomits repeatedly, retches without producing anything, has blood in the vomit, refuses food, seems weak, hides, appears painful, or has chronic recurring episodes, call your veterinarian.
Important Veterinary Note
This article is for general education only and cannot diagnose the cause of vomiting. Cat owners can observe shape, color, contents, timing, and behavior, but only a veterinarian can diagnose gastrointestinal disease, obstruction, pancreatitis, kidney disease, hyperthyroidism, toxin exposure, or other medical causes.
Call your veterinarian or an emergency clinic promptly if your cat vomits more than 2-3 times in 24 hours, retches without producing anything, vomits blood or coffee-ground material, refuses food, seems weak or painful, has diarrhea with vomiting, may have eaten string or a toxic substance, or is a kitten, senior cat, or cat with a known medical condition.
How to Check the Mess Before You Clean It
Let me walk you through exactly what goes through my mind when I encounter an unidentified feline deposit — because this diagnostic thought process is genuinely useful for every cat owner.
Step 1: Don’t Clean It Up Yet
I know. Every instinct screams grab the paper towels. Resist. What’s on your floor is clinical information. Take a photo with your phone first. If your cat starts vomiting frequently, that photo library becomes a valuable diagnostic timeline you can share with your vet.
Step 2: Assess the Shape
This is the single fastest differentiator in the cat vomiting vs hairball question:
- Cylindrical, elongated, tube-like: Almost certainly a Trichobezoar (hairball). The tubular shape is formed by compression inside the esophagus during expulsion.
- Formless puddle, splatter pattern, or foamy mound: This is vomit. The shape tells you it was propelled with force or contained mostly liquid content.
Step 3: Assess the Contents
Get close. Yes, really. This is what we do.
| What You See | What It Likely Means |
|---|---|
| Dense, matted fur — possibly mixed with a small amount of mucus | Classic Trichobezoar (hairball) |
| Recognizable kibble or wet food pieces, relatively undigested | Regurgitation or rapid vomiting shortly after eating |
| Yellow or green liquid | Bile — indicates the stomach was empty; potentially serious |
| Clear or white foam | Empty stomach vomiting; mucus-heavy; could signal reflux |
| Bright red streaks or coffee-ground appearance | Blood — this is an emergency |
| Brown liquid with foul odor | Possible lower GI involvement — emergency |
Step 4: Assess the Effort
Did you hear it happen? This matters enormously in the cat vomiting vs hairball distinction:
- Hairball expulsion typically involves a drawn-out, rhythmic retching sound — a repeated wretch-wretch-wretch that can go on for 30–60 seconds before the trichobezoar is expelled. Some cats crouch low during this process.
- Active vomiting is often more sudden, more forceful, and may involve a single heave or multiple rapid heaves in quick succession. The sound is different — more abrupt, more urgent.
Step 5: Assess Your Cat Immediately Afterward
This is perhaps the most important forensic step of all, and the one most owners skip.
A cat that just expelled a hairball will typically:
- Shake their head, sniff the result with mild curiosity
- Walk away looking entirely unbothered
- Return to normal behavior within minutes
- Show no signs of distress, lethargy, or appetite loss
A cat that is experiencing pathological vomiting may:
- Continue retching even after the stomach is empty
- Appear hunched, uncomfortable, or reluctant to move
- Refuse food or water
- Vocalize in distress
- Return to vomit again within the hour
The Oliver Test: The morning after my 2:47 AM encounter, Oliver was headbutting my ankle for breakfast by 6 AM as if nothing had happened. That behavioral normalcy told me everything I needed to know. It was a hairball. Case closed — until the next time.
The Anatomy of a Hairball (Trichobezoar)
Let’s talk about what a hairball actually is, because understanding the mechanism helps you recognize when something has gone wrong with the process.
What Is a Trichobezoar?
A Trichobezoar is a compacted mass of ingested hair that has accumulated in the stomach or esophagus. The word comes from the Greek tricho (hair) and the Persian padzahr (antidote/counter-poison) — bezoars were historically believed to have medicinal properties, which is a fun piece of trivia that has nothing to do with stepping on one at 3 AM.
Here’s how one forms:
- Grooming: A cat’s tongue is covered in backward-facing papillae — tiny, hook-like structures that are extraordinarily efficient at detangling fur. They are also extraordinarily efficient at directing every loose hair straight to the back of the throat.
- Ingestion: Most of that hair is swallowed. In the vast majority of cases, it passes through the digestive tract uneventfully and exits in the stool.
- Accumulation: When hair accumulates in the stomach faster than Gastric Motility (the natural muscular contractions that move content through the GI tract) can process it, it begins to compact.
- Expulsion: The body eventually triggers a vomiting reflex to expel the mass. The elongated, cylindrical shape is formed as the mass is compressed through the lower esophageal sphincter and esophagus on its way out.
Which Cats Are Most Prone?
- Long-haired breeds: Persians, Maine Coons, Ragdolls, Norwegian Forest Cats
- Heavy groomers: Particularly anxious or obsessive-compulsive groomers
- Cats with reduced Gastric Motility: Senior cats, cats with GI disease
- Multi-cat households: Some cats groom each other extensively (allogrooming)
- Seasonal shedders: Heavy hairball seasons correspond with spring and fall coat transitions
When Does a Hairball Become a Problem?
An occasional Trichobezoar — perhaps once or twice a month — is within the range of normal for a long-haired or heavy-grooming cat, though even this warrants dietary and grooming management.
It becomes a concern when:
- Your cat retches repeatedly without producing anything
- The cat appears distressed during or after the attempt
- Hairballs are occurring multiple times per week
- Your cat has lost interest in food around the time of hairball activity
- You notice constipation or reduced fecal output alongside hairball issues
If your analysis suggests a classic hairball and your cat is behaving normally, your next step is prevention. For a full grooming, diet, and monitoring plan, read our cat hairball prevention guide.
Prevention is harder if your cat fights the brush. If grooming is the main problem, use this alongside our indoor cat grooming guide so you can reduce swallowed fur without turning brushing into a battle.
5 Warning Signs That Vomiting Needs a Vet
This is the section I need you to read carefully. Distinguishing cat vomiting vs hairball isn’t just an academic exercise — it’s the difference between a “monitor at home” situation and a “rush to the emergency clinic” situation.
Here are the five red flags I look for as a veterinary technician:
Red Flag 1: Vomiting More Than 2-3 Times in 24 Hours
Frequency is your most reliable alarm bell.
An isolated vomiting episode — even one that doesn’t produce a hairball — is not necessarily cause for panic. Cats have notoriously sensitive stomachs, and a single episode of unexplained vomiting in an otherwise healthy, alert cat can sometimes be chalked up to eating too fast, dietary indiscretion, or mild gastric irritation.
But when vomiting occurs more than 2–3 times within a 24-hour window, the calculus changes entirely.
- Repeated vomiting rapidly depletes fluids and electrolytes
- It suggests active gastric or intestinal irritation rather than a one-time event
- It may indicate Intestinal Obstruction, toxin ingestion, or systemic disease
The rule I use in clinic: One episode — observe closely. Two or three episodes in the same day — call the vet and bring in a photo of the vomit. Four or more — this is a same-day appointment minimum, possibly an emergency visit.
Red Flag #2: Vomiting With No Production (Unproductive Retching)
If your cat is going through the full retching and heaving motion — back arching, neck extended, abdominal contractions — but producing nothing, this is a critical warning sign that demands immediate veterinary attention.
Unproductive retching can indicate:
- Intestinal Obstruction: A foreign body (string, toy piece, bone fragment) lodged in the GI tract. String foreign bodies are particularly catastrophic in cats — they can anchor at the base of the tongue and saw through intestinal tissue as the gut tries to move material past them.
- Gastric Dilatation: While far less common in cats than dogs, bloat-like presentations do occur
- A Trichobezoar too large to pass — requiring endoscopic or surgical removal
- Esophageal stricture or dysfunction
Do not confuse unproductive retching with the normal pre-hairball retching pattern, which typically resolves with expulsion within 60 seconds. Prolonged, repeated, unproductive retching is an emergency until proven otherwise.
Red Flag #3: Blood in the Vomit
There is no version of blood in vomit that is “probably fine.” Both presentations require prompt evaluation:
Bright red blood (hematemesis):
- Suggests active bleeding in the upper GI tract — esophagus, stomach, or upper small intestine
- Causes include ulceration, foreign body trauma, coagulopathy, or severe gastritis
Dark brown, “coffee-ground” material:
- Indicates digested blood — meaning the bleed is occurring higher in the GI tract and the blood has been partially broken down by stomach acid before expulsion
- This appearance is particularly associated with gastric ulceration
Either presentation warrants same-day emergency veterinary care.
Red Flag #4: Vomiting Accompanied by Lethargy, Fever, or Appetite Loss
Here is where the behavioral component of your forensic assessment becomes medically decisive.
A cat that vomits and then immediately returns to their normal routine — eating, playing, grooming, socializing — is exhibiting what we call a “vomit and recover” pattern. Concerning? Worth monitoring. An emergency? Usually not.
A cat that vomits and then:
- Refuses food or water for more than 12–24 hours
- Becomes lethargic, withdrawn, or difficult to rouse
- Feels warm to the touch (fever) or unusually cold
- Stops grooming
- Hides persistently
…is telling you something is systemically wrong. This combination of vomiting with systemic illness signs is a red flag for conditions including pancreatitis, liver disease, sepsis, viral illness, or toxin ingestion.
A note on senior cats: if an older cat starts vomiting more often, do not assume it is normal aging or stress. Recurring vomiting can overlap with appetite changes, weight loss, confusion, hiding, or other behavior shifts. For behavior changes in older cats, read our guide to senior cat dementia signs, but vomiting itself should still be discussed with your veterinarian.
As cats age, cognitive decline and feline cognitive dysfunction can contribute to stress-induced GI upset, altered eating patterns, and vomiting that owners may dismiss as “just hairballs” or aging. If your senior cat is showing unusual vomiting patterns alongside behavioral changes, please read our guide on feline cognitive dysfunction before assuming the cause is benign.
Red Flag #5: Chronic, Recurring Vomiting (More Than Once a Week for Multiple Weeks)
This is the red flag that gets missed most often, because each individual episode seems manageable. A vomit here, a vomit there — owners adapt and normalize it over weeks and months.
Chronic vomiting is never normal, even when the individual episodes seem mild.
Conditions that present as chronic, recurrent vomiting include:
- Inflammatory Bowel Disease (IBD): Chronic inflammation of the GI tract; highly prevalent in middle-aged to senior cats
- Alimentary lymphoma: Gastrointestinal cancer that can mimic IBD clinically
- Chronic kidney disease (CKD): waste products can build up and irritate the digestive tract. If vomiting appears with weight loss, appetite changes, increased thirst, or more urination, review these chronic kidney disease cats signs and ask your vet about bloodwork and urinalysis.
- Hyperthyroidism: Elevated thyroid hormone accelerates
- Gastric Motility to the point of chronic gastric irritation
- Exocrine pancreatic insufficiency: Inability to produce digestive enzymes leads to chronic GI upset
The distinction between cat vomiting vs hairball becomes most critical in these chronic cases. Every week of missed diagnosis is another week of disease progression.

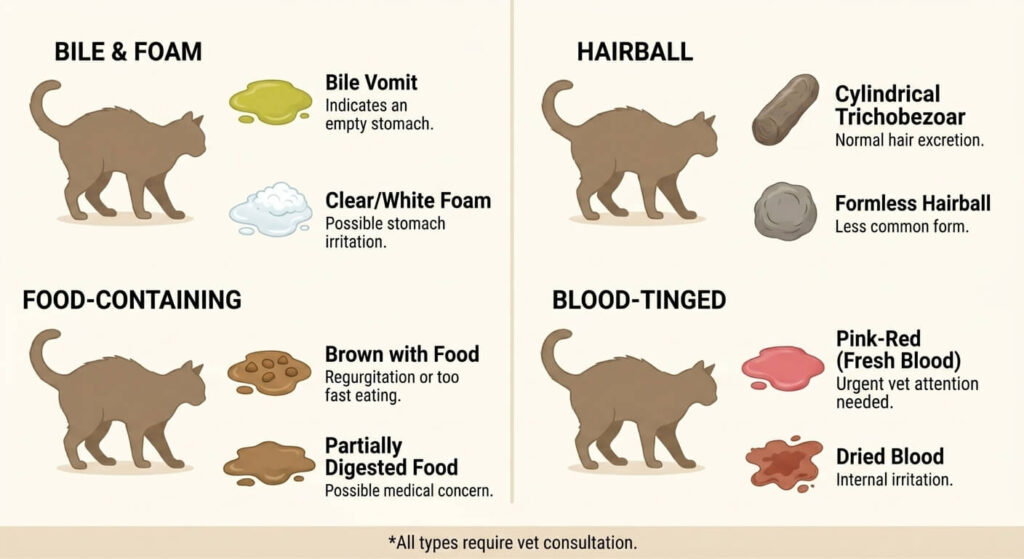
The Color Code: What Yellow, Clear, and Bloody Vomit Mean
Color is one of the most information-dense diagnostic clues in the cat vomiting vs hairball assessment. Here’s your quick-reference color decoder:
Yellow or Green Vomit = Bile
What it is: Bile is a digestive fluid produced by the liver and stored in the gallbladder. It enters the small intestine to aid fat digestion. When a cat vomits on an empty stomach, bile from the upper small intestine can be refluxed into the stomach and expelled.
What it means:
- The stomach was empty at the time of vomiting
- May indicate “hunger pukes” in cats fed once daily (simply feed more frequently)
- May indicate bilious vomiting syndrome — chronic reflux of bile into the stomach
- In a sick cat, bile-colored vomit suggests the GI tract has been purged of food content — a sign of more significant illness
When to worry: Yellow vomit once in a hungry cat — monitor. Yellow vomit repeatedly in a cat that has been offered food and is lethargic — same-day vet call.
Clear or White Foam = Empty Stomach / Mucus
What it is: Clear liquid vomit or white foam represents stomach secretions, mucus, and saliva — essentially, what’s left when there’s nothing else to bring up.
What it means:
- Stomach was completely empty
- Can be normal in a cat that has already purged food content
- White foam can precede hairball expulsion — the foam lubricates the passage
- Persistent clear/foam vomiting can indicate gastric reflux, esophagitis, or early systemic illness
Brown, Food-Containing Vomit
What it is: Recently consumed food or food that has partially begun to digest.
What it means:
- Undigested kibble shortly after eating: Likely regurgitation (esophageal, not stomach-based) or eating too fast. Try puzzle feeders or slow-feed bowls.
- Partially digested food hours after eating: Delayed gastric emptying, gastritis, or Gastric Motility disorder
- Dark brown with foul odor: Potentially indicates a lower GI issue — seek immediate care
Pink, Red, or “Coffee Ground” = Blood
As discussed in Red Flag #3 — any visible blood in vomit is a veterinary emergency without exception.
Green Vomit
Less common than yellow, but green coloration can indicate:
- Bile with additional digestive enzyme content
- Ingestion of grass or plant material (common and usually benign if isolated)
- In persistent cases — upper intestinal content reflux
The Hairball Color Profile
For comparison: a classic Trichobezoar is typically:
- Brown to gray in color (reflecting the cat’s coat color and stomach content)
- Cylindrical and firm with visible hair texture
- Sometimes surrounded by a small amount of clear or slightly yellow mucus
- Not liquid — if it’s primarily liquid with some hair mixed in, that’s vomit, not a hairball
The Frequency Rule: Normal Cat Vomiting vs Hairball Patterns
This is perhaps the most contested question in the entire cat vomiting vs hairball discussion, because for years — decades — veterinary culture and popular cat ownership culture held the same convenient assumption:
“Cats vomit. It’s just what they do.”
I am here to firmly retire that idea.
The Myth of the “Vomiting Cat”
The normalization of feline vomiting has caused immeasurable harm. It has led countless owners to watch their cats slowly deteriorate from IBD, CKD, hyperthyroidism, and alimentary lymphoma — dismissing each episode as “just a hairball” or “just their sensitive stomach” — until the disease was in an advanced, harder-to-treat stage.
The current veterinary consensus, supported by the ISFM and WSAVA GI guidelines, is this:
A healthy cat should not vomit regularly. Any vomiting pattern that occurs more than once or twice per month warrants veterinary investigation.
The Frequency Framework
| Frequency | Category | Action |
|---|---|---|
| Once, cat acting totally normal | Isolated episode | Monitor closely for 24 hours |
| 2–3 times in one day | Acute episode | Call your vet; same-day if possible |
| More than 3 times in one day | Acute emergency | Emergency clinic |
| Once a week or more, recurring | Chronic vomiting | Veterinary workup required |
| Once or twice a month | Borderline | Discuss with vet at next visit; investigate diet |
| Once a month, long-haired cat, confirmed trichobezoar | Possible normal with prevention | Implement hairball prevention protocol |
The “Vomit Diary” Approach
I recommend this to every owner who tells me their cat “vomits sometimes.” For two weeks, keep a simple log:
- Date and time of each episode
- Description: Contents, color, shape, volume
- Before/after behavior: Was the cat acting normally?
- Feeding details: What was fed, when, how much
- Photo if possible
This data transforms a vague “vomits sometimes” into a diagnostic picture your veterinarian can actually work with. It’s saved multiple cats I know of from months of missed diagnosis.
You can also pair the diary with a simple monthly cat health check at home, especially if your cat is senior, losing weight, drinking more, or acting differently between vomiting episodes.
A Note on the Cat Vomiting vs Hairball Frequency Distinction
In the frequency context:
- Hairballs in long-haired cats: Up to 1–2 per month with confirmed Trichobezoar production and normal behavior may be manageable (though still worth addressing with prevention strategies)
- Vomiting in any cat, any frequency beyond once monthly: Never normalize it
The moment you catch yourself saying “Oh, she just does that” — that’s the moment to make a vet appointment.
Frequently Asked Questions
Why Is My Cat Vomiting But Acting Normal?
This is one of the most common questions in the cat vomiting vs hairball space, and the answer is nuanced.
Cats that vomit but appear immediately normal afterward are most commonly experiencing one of the following:
- A hairball expulsion: The most benign explanation — once the Trichobezoar is out, the cat feels immediate relief and returns to normal
- Eating too fast: Rapid eating causes food to be poorly mixed with gastric acid; the stomach reflexively ejects it. Gastric Motility is otherwise normal.
- Dietary indiscretion: The cat ate something irritating — grass, a small piece of something off the floor, a food they’re mildly sensitive to
- Mild reflux: Occasional gastric reflux can cause a single vomiting episode without systemic illness
When “acting normal” isn’t reassuring enough:
Even if your cat bounces back quickly, frequent vomiting — even in a cat that seems fine otherwise — warrants investigation. IBD and alimentary lymphoma, in particular, are notorious for allowing cats to maintain relatively normal behavior in the early stages while pathology progresses silently. “Acting normal” tells you about today. It doesn’t tell you about the state of the intestinal villi or the kidney function.
Bottom line: One episode, normal behavior → monitor. Recurring episodes, normal behavior between them → schedule a workup.
Should I Withhold Food After My Cat Vomits?
Short answer: For a brief period, yes — with important caveats.
The traditional approach: After a single vomiting episode, many veterinarians recommend:
- Withholding food for 2–4 hours to allow gastric irritation to settle
- Offering small amounts of water (or ice cubes for cats that drink slowly)
- After the fast period, offering a small amount of bland food — plain boiled chicken, a teaspoon of prescription GI food — and observing the response
- Gradually returning to normal feeding if no further vomiting occurs
When NOT to withhold food:
- Diabetic cats: A diabetic cat cannot fast safely — hypoglycemia risk is significant. Call your vet for specific guidance.
- Kittens: Young cats have very limited glycogen reserves; extended fasting is dangerous
- Cats that haven’t eaten in 24–48 hours already: Fasting further risks hepatic lipidosis (fatty liver disease), a serious and potentially fatal condition in cats
- Any cat showing signs of systemic illness: These cats need veterinary assessment, not home fasting protocols
Never fast a cat for more than 12–24 hours without veterinary guidance.
Is White Foam a Sign of a Hairball?
Yes — sometimes. But it’s also very frequently not.
White foam vomit can precede hairball expulsion, because the body produces mucus to lubricate the esophagus in preparation for Trichobezoar passage. If you hear that characteristic rhythmic retching, see white foam produced, and then a cylindrical fur mass follows — that’s a hairball sequence.
However, white foam vomit that occurs:**
- Without a subsequent hairball
- Repeatedly throughout the day
- In a cat that is also lethargic or anorexic
- In a cat not known to be a heavy groomer
…is not a hairball. White foam as an isolated, recurrent finding is associated with:
- Empty stomach reflux / bilious vomiting syndrome
- Pancreatitis
- Esophagitis
- Early kidney disease (the uremic environment irritates the gastric lining)
- Inflammatory Bowel Disease
- Hairball obstruction (the body is trying to expel something it cannot)
The key question to ask: Did a Trichobezoar follow the foam, and did the cat immediately return to normal behavior? If yes — hairball. If no — investigate further.
Final Thoughts
Cat vomiting vs hairball questions are common because the signs can look similar in the moment. The safest approach is not to guess from one clue alone. Look at the shape, contents, color, effort, frequency, and your cat’s behavior afterward.
A single firm hairball in a cat who immediately returns to normal is very different from repeated vomiting, unproductive retching, blood, lethargy, appetite loss, or chronic recurring episodes. When in doubt, take a photo, write down the timing, and call your veterinarian.
The goal is not to panic over every mess on the floor. The goal is to notice the pattern early enough that a medical problem does not get dismissed as “just fur.”
Scientific References
- Cannon, M. (2013). Hair balls in cats: A normal nuisance or a sign that something is wrong? Journal of Feline Medicine and Surgery, 15(1), 21–29. https://doi.org/10.1177/1098612X12472177
- Jergens, A. E., & Simpson, K. W. (2012). Inflammatory bowel disease in veterinary medicine. Frontiers in Bioscience (Elite Edition), 4, 1404–1419. https://doi.org/10.2741/e470
- Cornell Feline Health Center. Vomiting. Cornell University College of Veterinary Medicine.
- Merck Veterinary Manual. Vomiting in Cats.
- VCA Animal Hospitals. Vomiting in Cats.
- VCA Animal Hospitals. Trichobezoars in Cats. https://vcahospitals.com/know-your-pet/trichobezoars-in-cats
- Cannon, M. (2013). Hair balls in cats: A normal nuisance or a sign that something is wrong? Journal of Feline Medicine and Surgery, 15(1), 21-29. https://doi.org/10.1177/1098612X12472177

-300x169.png)
-300x169.png)
